Dr. Gary Landreth and colleagues at Case Western Reserve published a paper online in Science Express yesterday that received much attention because of the rather stunning results it reports in stopping and even reversing “a broad range of Abeta-induced deficits.”
A good lay version of this, with comments from Cure Alzheimer’s Fund–supported researchers Sam Gandy of Mount Sinai Medical School and David Holtzman of Washington University in St. Louis can be found in the Feb. 9 edition of the Huffington Post Healthy Living section online here.
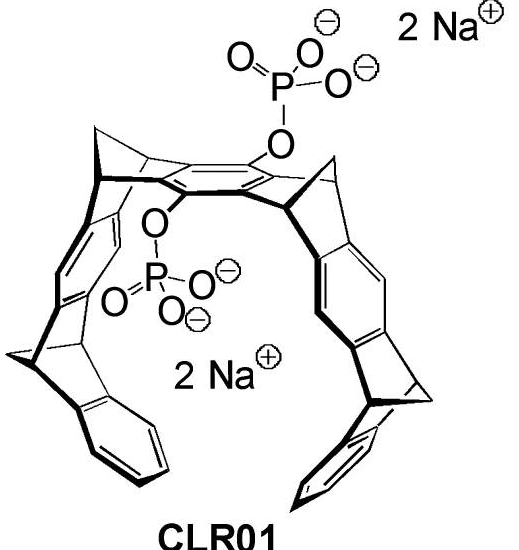
Cure Alzheimer’s Fund participated in the early stage funding of this work that focuses on the drug Bexarotene (marketed under the name Targretin), which was developed more than ten years ago for a specific kind of lymphoma. In laboratory trials with mice, the drug appeared to significantly improve clearance of the Abeta peptide, which is widely believed to play a key role in Alzheimer’s pathology.
Clearance of Abeta is largely the job of a gene called APOE, although its variant APOE4 is thought to inhibit clearance and therefore promote build-up of the Abeta peptide conferring a much higher risk for the disease. In laboratory trials, the drug seems to block the negative effects of APOE4 and enhance the clearance capabilities of APOE, thus causing reversal of cognitive deficits and pathological features with remarkable speed.
This work is important for at least two reasons. First, it reinforces the importance of the APOE gene family in both lowering risk for Alzheimer’s (APOE 2 and 3 promote clearance) and increasing risk for the disease from the APOE4 gene variant. Secondly, the work offers a new and possibly much more immediate way to interrupt the pathology.
However, as the Huffington article points out and as researchers constantly remind us, moving from “mice to men” is a big leap that requires more careful and expensive research. Bexarotene is now being considered for human trials for effectiveness and safety at the effective doses.
Although the drug is available now for lymphoma patients, Dr. Landreth echoes the cautionary concerns of most researchers saying, “Don’t try this at home…because we don’t know what dose to give, we don’t know how frequently to give it, and there are a few nuances to its administration. So one shouldn’t be prescribing it off-label.”
It is a big step on the research process, but it is definitely NOT ready for the clinic.
We congratulate Dr. Landreth and his colleagues on this progress and look forward to results from human clinical trials.
Please read this update on Targretin from May 2013.