Research suggests Abeta is an antimicrobial peptide and that infection may trigger plaque buildup in the brains of Alzheimer’s patients
Wellesley, Mass. (May 25, 2016) – A key protein found in the brain of Alzheimer’s disease patients is related to the body’s innate immune system – raising new questions about the role of infection in Alzheimer’s disease, according to research published in Science Translational Medicine and funded by Cure Alzheimer’s Fund.
The protein, amyloid beta (Abeta), makes up the plaques in the brain associated with Alzheimer’s patients. The study suggests that Abeta is an antimicrobial peptide, a critically important protein that acts as a natural antibiotic in the immune system. The study raises new implications about the potential role of pathogens in Alzheimer’s disease, and potential avenues for treatment.
The findings are detailed in a new paper, “Amyloid-beta peptide protects against microbial infection in mouse and worm models of Alzheimer’s disease,” co-authored by Robert Moir, Ph.D., assistant professor of neurology at Harvard Medical School and Massachusetts General Hospital Neurology Research, and Rudolph Tanzi, Ph.D., vice-chair of Neurology and director of the Genetics and Aging Research Unit at MGH and Joseph P. and Rose F. Kennedy Professor of Neurology at Harvard Medical School. Dr. Tanzi is the chair of the Cure Alzheimer’s Fund Research Consortium.
“Abeta was previously thought to be intrinsically pathological, but our findings suggest it is actually designed to protect the brain,” said Dr. Moir. “Because of Abeta’s role as part of the innate immune system, researchers may need to more carefully consider infection as a possible environmental factor leading to the development of Alzheimer’s.”
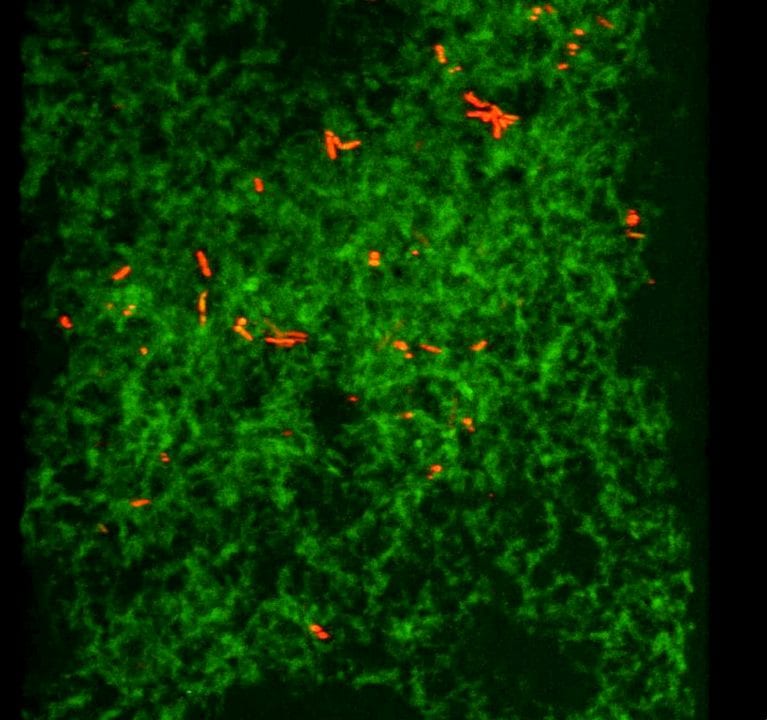
In the study, human Abeta protected against otherwise lethal infections in mice, nematode worms and cultured neuronal cells. In addition, Abeta generation appears to have a protective physiological role, entrapping invading pathogens in a degradation-resistant protein matrix.
The findings support a new anti-microbial protection hypothesis: Alzheimer’s disease may arise when the brain perceives itself to be under attack from invading pathogens and launches Abeta formation. Additional study is needed to determine whether Abeta is responding to actual or perceived infection in the brains of Alzheimer’s patients.
As people age and their adaptive immune system changes, they may become more susceptible to pathogens that enter the body.
The study may also have implications for Alzheimer’s therapies currently in development, which are largely based upon the premise that Abeta is pathological. Instead of eradicating the protein from the brains of Alzheimer’s patients, a safer approach may be therapies that are designed to lower Abeta levels without destroying them entirely.
“The finding of an innate immune role for Abeta activities shows a clear and urgent need to review the assumptions currently guiding efforts to develop treatments for this terrible disease,” said Dr. Tanzi.
The study, which was published online in Science Translational Medicine, was funded by Cure Alzheimer’s Fund and the National Institute on Aging. Cure Alzheimer’s Fund provided $1.6 million in funding, made possible in part by a grant from the Helmsley Foundation.
“This research offers a major paradigm shift when it comes to Abeta and the important role it plays in the immune system,” said Timothy Armour, president and CEO of Cure Alzheimer’s Fund. “Not only do these findings raise questions about the potential causes of Alzheimer’s, but they generate new avenues of inquiry into the therapies that may best target the disease.”
About Cure Alzheimer’s Fund
Cure Alzheimer’s Fund is a non-profit dedicated to funding the most promising research to prevent, slow or reverse Alzheimer’s disease. Since its founding in 2004, Cure Alzheimer’s Fund has contributed over $40 million to research, and its funded initiatives have been responsible for several key breakthroughs – including the groundbreaking “Alzheimer’s in a Dish” study. With 100 percent of funds raised going directly to research, Cure Alzheimer’s has been able to support some of the best scientific minds in the field of Alzheimer’s research. For more information, please visit curealz.org.