Finding the correct arsenal for preventing plaques, tangle formation and neuroinflammation is the holy grail for scientists studying Alzheimer’s disease. All three join together to disrupt communication between neurons—leading to an eventual complete loss of autonomy.
The Newfound Focus on Tau
Plaques are composed of amyloid protein and have been the major focus of Alzheimer’s research for the past decade or so. In contrast, tangles, which are composed of the protein tau, have garnered much less attention. Clinical trials aimed at combating amyloid offer some hope, but results have been disappointing, and although there are many amyloid drugs still being developed and tested, scientists are widening their focus to include more investigations of tau. Some of this newfound excitement stems from newly marketed chemical compounds that, when injected by IV, attach to tau in the brain, allowing patterns of its accumulation to be imaged through positron emission tomography (PET) in living people. Analogous chemicals that bind to amyloid have been in use for several years and have greatly helped to improve the patient selection process for clinical trials. These brain imaging techniques that localize and quantify both amyloid and tau help fuel promising research. Tau imaging studies consistently report that the progression of tau closely tracks with the progression of cognitive decline, which is not the case for amyloid. Thus, investigating tau’s properties, such as how tangles form and then spread, can inform drug discovery.
Tangles develop after amyloid builds up, and once tangles form, they seep into brain structures along a predictable path. They travel from their initial site in the medial temporal lobe (the brain’s memory center), eventually ending up in the neocortex (the brain’s outer layer), which is responsible for complex forms of cognition such as reasoning. Amyloid buildup sends an incompletely understood set of signals that encourage tau to change shape and to form tangles. These tangles, along with plaques, clog the system, leading to eventual cognitive decline.
Alzheimer’s Disrupts Tau Clearing Process
In Alzheimer’s disease, systems that promote clearance of extraneous proteins like amyloid and tau can malfunction. One such protein-clearing system is the ubiquitin-protease system (UPS)—the current focus of an investigation being led by Karen Duff, Ph.D., and Natura Myeku, Ph.D., at Columbia University through a grant provided by Cure Alzheimer’s Fund. The UPS is responsible for maintaining proper protein balance within cells. Ubiquitin binds to proteins, tagging them for destruction. When the proteasomes within the UPS find the tags, they swallow the proteins. However, when this system is up against the likes of Alzheimer’s disease, it can be overpowered, begin to fizzle out and lose its ability to clear unwanted tau protein. Once this deleterious sequence is set in motion, tau can spread.
Resurrecting Tau Clearance
Duff and Myeku now are investigating whether drug therapy aimed at resurrecting the UPS system by kickstarting proteasomes can bring tau spread to a halt. If Duff and Myeku find a drug effective at stopping tau spread in mice, the hope is that it can be harnessed for therapeutic development in humans.
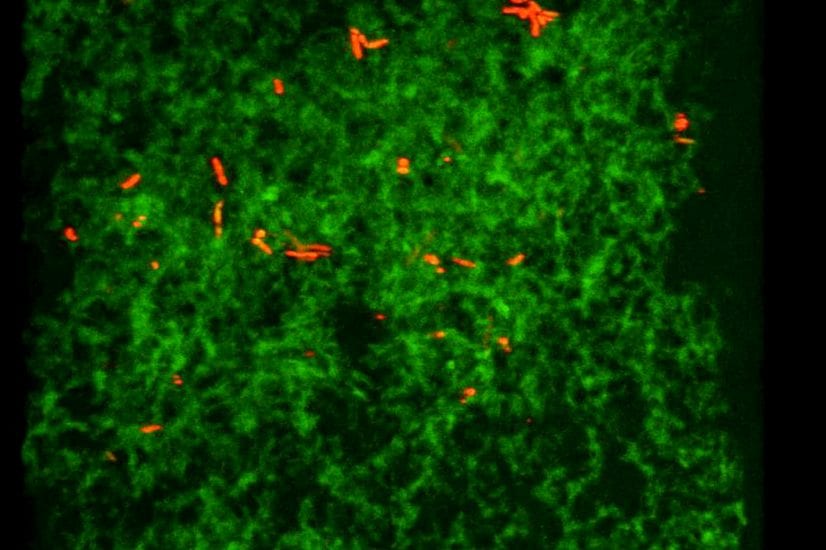
How will they do it? They will invoke tangle formation by introducing a human form of tau into the entorhinal cortex—the initial site of tau formation. Using a fluorescent tracer that highlights proteins in the UPS, they will be able to visualize where in the brain the tau has traveled. Using other tissue-examination methods, they also will be able to tell more specifically what compartments within the neuron (e.g., dendrite, axon) are contaminated with misfolded tau.
The next step is to try to prevent tau spread through drug therapy. They are pioneering a method in which a chemical compound will be injected locally, at the initial site of tau formation. Myeku explains that “The goal is to eventually use drugs in the synapse, where tau gets transferred from one neuron to another.” Duff adds, “Placing a drug in the precise place where tau is doing its damage will have the most impact.”
The compound Duff and Myeku are using works by restoring function to the proteasome to enable protein clearance. Additionally, its target is very specific, acting on just the portion of the neuron where tau initiates—where it can do the most good.
The very real possibility of being able to clear tangles raises the question of what symptoms will look like if the tau problem is solved before the amyloid one. “Finding a drug that can remove tangles, even if amyloid remains, will greatly decrease cognitive dysfunction and improve quality of life. There will still be cognitive problems, but they will be far reduced,” explains Duff.
Armed with a drug that can remove tau, techniques like PET imaging that visualize tau and amyloid in a human patient can be harnessed to tailor therapies that match the level of the individual patient’s disease. “PET imaging can show you where the amyloid and tau have traveled—and that information is critical, especially for tau, as its spread tracks so closely with disease symptoms. We are in very exciting times as we approach a point where we can position our drug toolbox to select the right treatment for the right patient,” concludes Duff.